When Dispatch launched last year, we did so with an investigation into Britain's hidden opioid crisis. Using Freedom of Information requests, we revealed for the first time the geographical spread of a new class of synthetic drugs: nitazenes, which can be 500 times stronger than heroin.
We charted their arrival in Britain in 2023, and tried to understand why Birmingham, in particular, was so badly hit. The answer, as so often with public-health disasters, lay in a tangle of missed warnings, bad luck and political dysfunction.
The story did not disappear after publication. Our reporting was picked up by national newspapers, magazines and broadcasters. The UK Border Force began training dogs to detect nitazenes. Local councils started distributing opioid-reversing naloxone kits. The Home Secretary Shabana Mahmood convened an international summit to discuss the growing threat posed by synthetic opioids.
It was easy, watching all this, to feel that something was being done.
But was it?
Today, Dispatch can reveal that Britain's opioid crisis has not been contained, but has instead continued to grow. New regions are in the grip of synthetic drugs; the compounds themselves are mutating; and obtaining them, we found, requires nothing more sophisticated than a WhatsApp message.
Most alarming of all, however, is the extent to which the state still lacks even the most basic understanding of what is happening. A year on from our original report, the task of monitoring deaths from synthetic opioids is not being led by a government agency or a specialist public health team, but by a single researcher at King's College London who is running a laboratory funded with her own money.
Her name is Caroline Copeland, and despite the fact that this isn’t her primary job, she continues to make important discoveries of national significance. Chief among them: that Britain is dramatically undercounting the true number of deaths caused by synthetic opioids.
Before we get to that, it is worth taking stock of how the landscape has shifted over the past year.
Last year, we sent FoI requests to every ambulance service in the UK, asking how many patients were treated with naloxone, the drug used to rapidly reverse an opioid overdose, in each local authority district in 2024. The methodology has its limits. Paramedics tend to reach for naloxone when they suspect any drug overdose, not only opioid ones, and the data doesn’t capture the increasing number of overdoses treated outside ambulance services: such as by outreach workers, family members or strangers.
But in the absence of reliable national data — and with the government’s own dashboard described by insiders as “useless” and missing large swathes of information — it is one of the few ways to trace and compare overdose trends across the country.
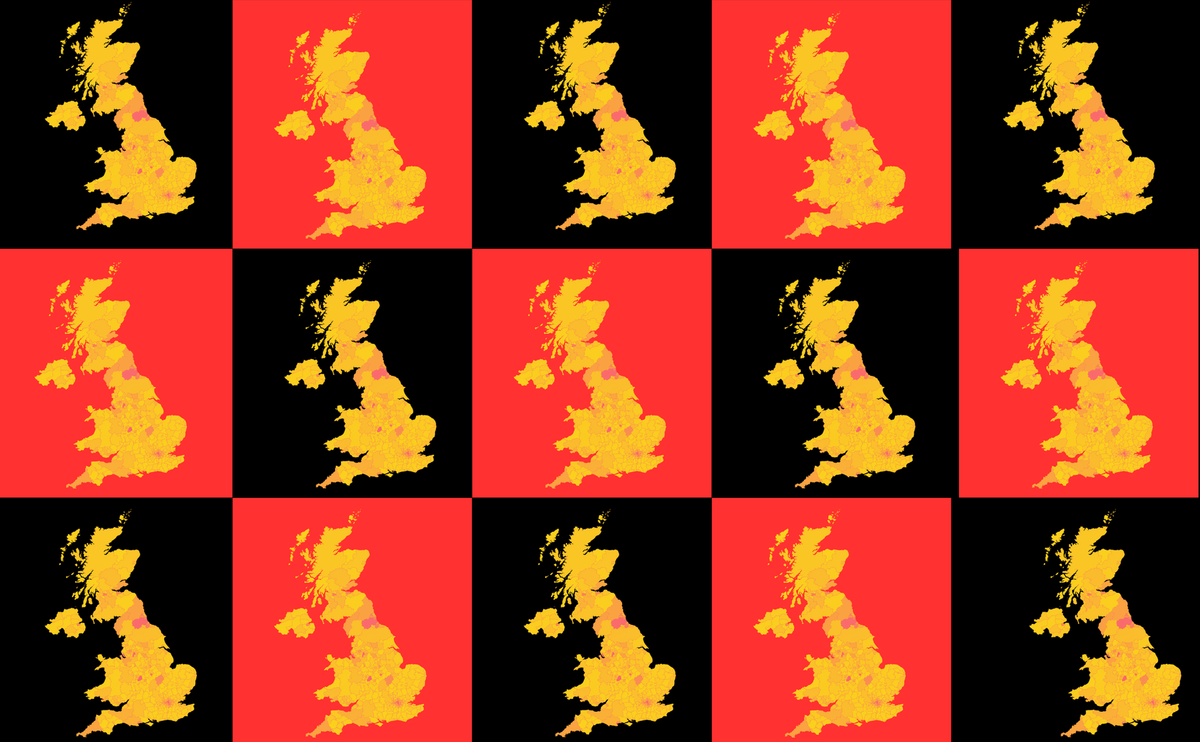
The data for 2024, illustrated on the below map, revealed a crisis concentrated in a handful of cities: Birmingham, Glasgow, Leicester, and Belfast.
What changed in 2025?
Compare the above map with the below. In general, there is a lot more blue, indicating a widespread increase in opioid overdoses across the UK.
There have been some decreases — in notable hotspots such as Birmingham, Leicester and Glasgow — but they are the exception, and their numbers still remain high.
Elsewhere, Manchester, County Durham, Camden, Liverpool and Newcastle have all recorded striking increases. Cornwall, badly hit in previous years, remains on the front line.
Register for free to read this article.